NON-TUMORAL CAUSES OF PULSATILE TINNITUS Arterial causesĪn aberrant carotid artery results from abnormal regression of the cervical segment of the embryonic ICA, necessitating development of a collateral pathway to provide vascular supply to the developing brain. Avid enhancement of the solid portions of the tumor is noted on post-contrast studies. Multiple high-signal intensity foci on both T1- and T2-W images may be due to blood products, proteinaceous cysts, or cholesterol clefts. On MRI, the ELSTs usually have a heterogeneous appearance with cystic components. Familial paragangliomas constitute approximately 10% of cases but have a higher incidence of multicentric tumors, being seen in 35–50% of cases. Multicentricity is seen in 10% of paragangliomas. MRI is superior to CT in showing the location and extent of these tumors and relation to adjacent vascular structures to assess operability. MRI may reveal a characteristic “salt and pepper” appearance on both T2 weighted (T2W) and post-contrast T1W images. 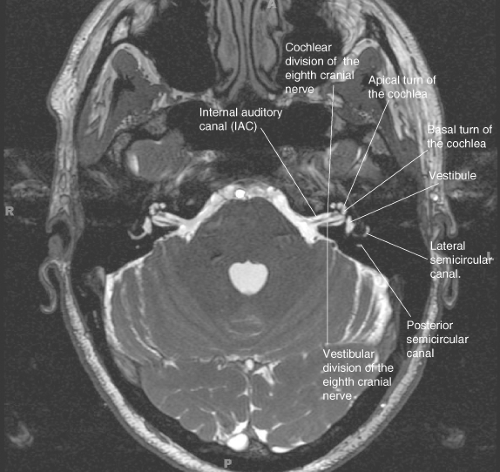
Intense homogenous enhancement is seen on the contrast enhanced CT scan. Intracranial or infratemporal fossa involvement again may occur in advanced tumors. Middle ear invasion with destruction of ossicular chain and adjacent bony landmarks may occur with larger lesions. On CT, irregular moth-eaten cortical erosions and widening of the jugular foramen are typical. Glomus jugulare tumors arise primarily in the jugular fossa while glomus jugulotympanicum involves both jugular bulb and middle ear cavity. However, most small tumors can be reliably evaluated on thin-section CT alone. These tumors enhance brilliantly on the post-contrast MRI images. Larger tumors may encase the ossicular chain without destruction. These tumors are variable in size and usually present as a small soft-tissue nodule classically located at the cochlear promontory, though occasionally, the tumor may be large enough to fill the tympanic cavity and extend posteriorly into the mastoid or anteriorly in to the Eustachian canal and nasopharynx. Glomus tympanicum arises in the middle ear from the paraganglia along Jacobson’s nerve near the cochlear promontory. Besides PT, hearing loss, vertigo, and symptoms related to adjacent cranial nerve involvement (CN IX–XI) may be noted. Both glomus jugulare and glomus tympanicum tumors have a predilection for females (F:M: 3:1) in fifth and sixth decades of life. 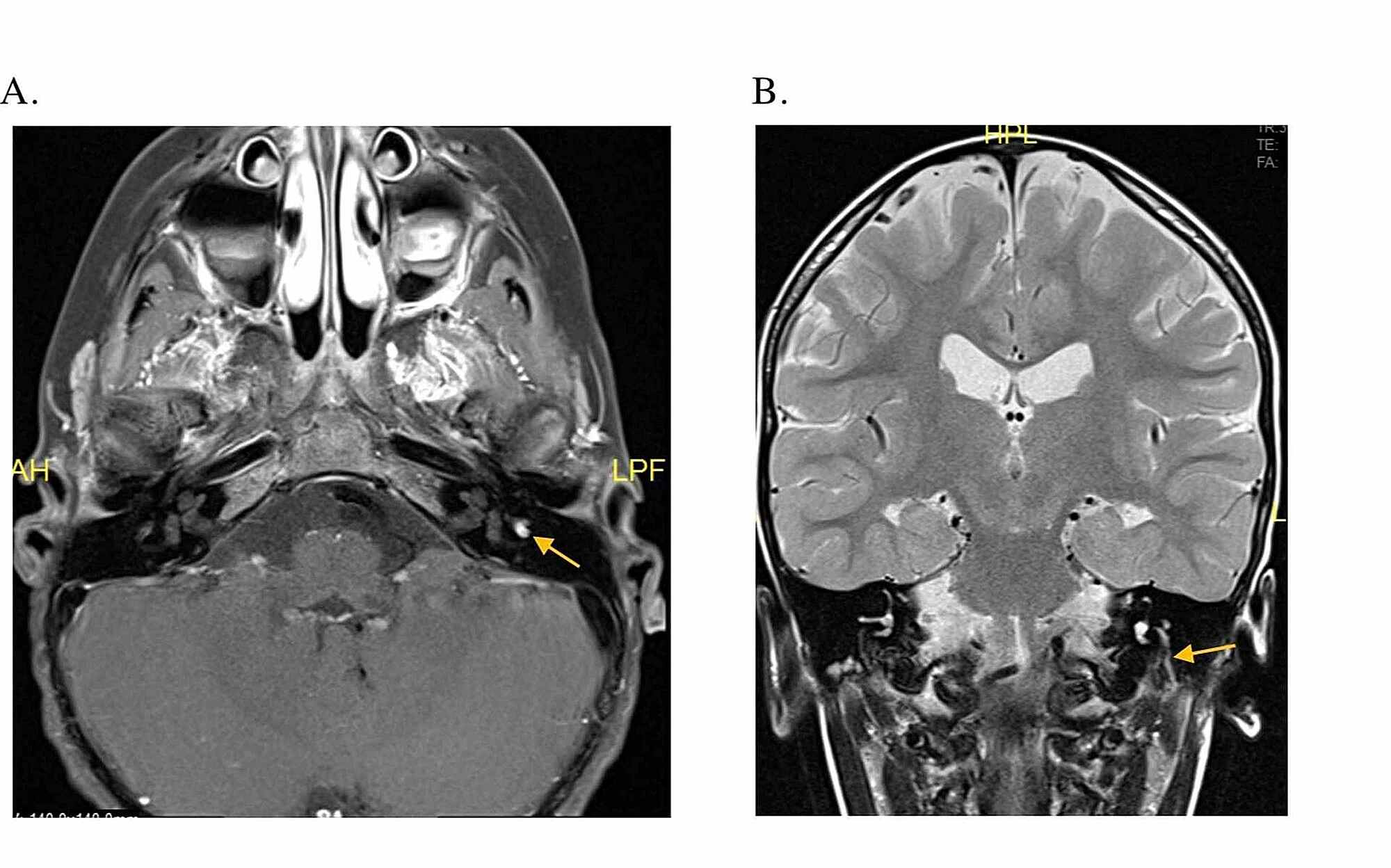
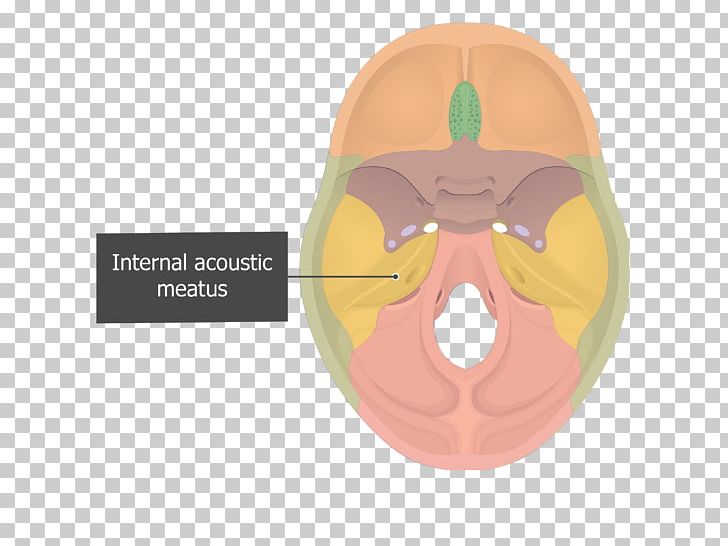
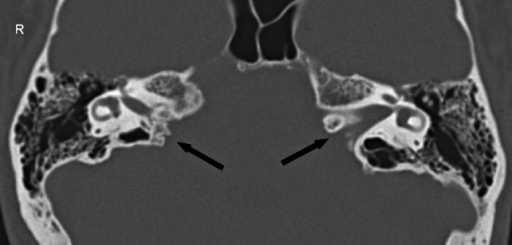
These tumors may arise from the middle ear cavity (glomus tympanicum), jugular bulb (glomus jugulare) or may involve both the jugular bulb and middle ear cavity (glomus jugulotympanicum). Glomus tumors/paragangliomas of the temporal bone arise from glomus cells that accompany tympanic branch (Jacobson’s nerve) of the glossopharyngeal nerve and the auricular branch (Arnold’s nerve) of the vagus nerve. In patients with PT, however, imaging may be positive in up to 57–100% of patients though about 20–30% of these patients have “normal variants” of controversial significance. Most patients with isolated non-PT do not show any significant abnormality on imaging. CT angiography/venography or conventional angiography is used to demonstrate dural fistula and other rarer venous causes of tinnitus on patients in whom the initial workup is unyielding. For a patient with a normal otologic examination or with no abnormalities on HRCT, an magnetic resonance imaging (MRI) examination and an magnetic resonance angiogram (MRA) are obtained to evaluate for causes related to common carotid artery disease, ICA disease, and benign intracranial hypertension. Aberrant or lateralized internal carotid artery (ICA), persistent stapedial artery (PSA), high-riding jugular bulb, glomus tympanicum, or cholesteatoma are the best demonstrated on computed tomography (CT). High-resolution computed tomography (HRCT) of temporal bone with contrast is the preferred modality, more so if a retro tympanic mass is seen on the otological examination. Non-vascular causes of PT include lesions of middle ear, temporal bone, internal auditory canal (IAC), and cranial cavity. PT may result from an underlying vascular tumor, a vascular malformation or etiology, developmental abnormalities, and in systemic conditions associated with high cardiac output. MRI: Magnetic resonance imaging, ICA: Internal carotid artery, CT: Computed tomography, MRA: Magnetic resonance angiogram, AV: Arteriovenous, IIH: Idiopathic intracranial hypertension 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
